

Cervical cancer is one of the most treatable cancers, especially when detected early. Gynaecologists can develop effective treatment plans based on factors such as the stage of the cancer, the patient's overall health, and individual preferences, such as preserving fertility.
This is generally regarded as a more extensive form of a typical cervical biopsy—a cone-shaped wedge of abnormal cervical tissue will be removed from the cervix and sent for examination. A cone biopsy is usually used to remove abnormal tissue high in the cervical canal. In most cases, this procedure is performed in the clinic as an outpatient day-surgery procedure under local anaesthesia. It is rarely necessary to have a general anaesthesia. A cone biopsy can be used for both diagnostic and treatment purposes, as abnormal cervical tissue is removed.
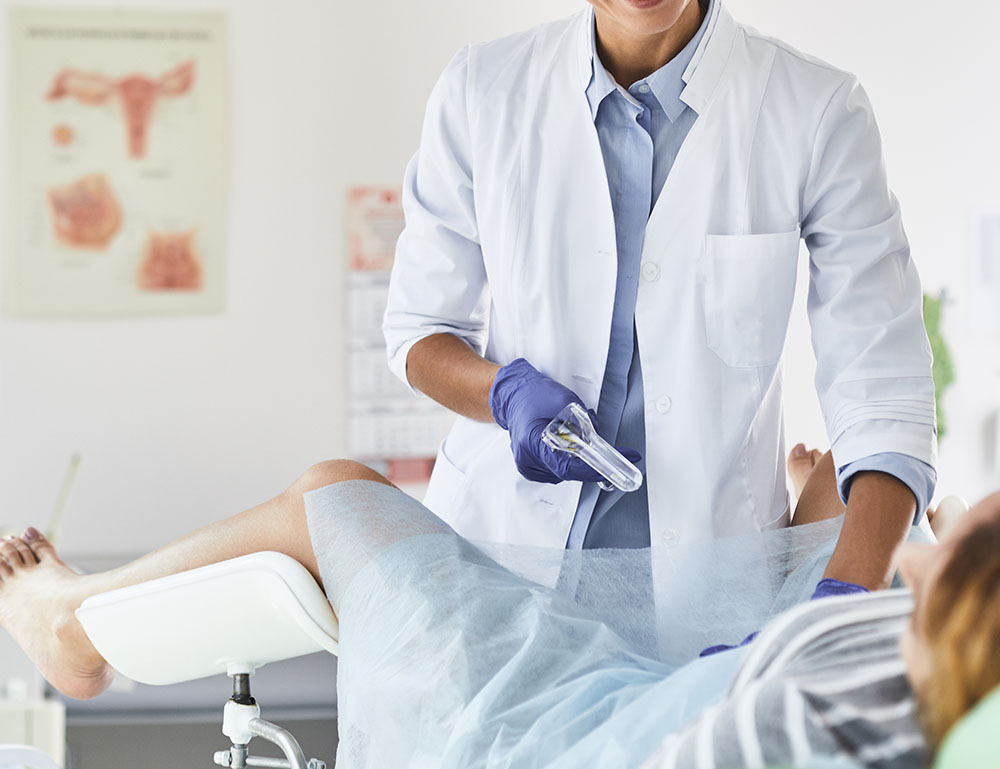
LEEP (Loop Electrosurgical Excision Procedure)—also known as LLETZ (Large Loop Excision of the Transformation Zone)—is a method of removing abnormal tissue growths in the cervix called cervical intraepithelial neoplasia (CIN). With local anaesthetic, an electrically charged wire loop is used to remove the abnormal cells, and bleeding is stopped with electrocautery and/or the application of Monsel’s solution. LEEP/LLETZ is also one of the most commonly used methods to treat high-grade cervical dysplasia (CIN2 and CIN3) discovered during a colposcopic examination.
A laser can be used to treat pre-cancerous and other conditions in the cervix. Due to its precision, this method is usually used during the pre-cancerous and early stages of cervical cancer, involving a focused carbon dioxide laser beam to burn off or cut off the abnormal cells in the cervix.
In many cases of precancer (CIN 2-3), the disease only involves the outer part of the cervix and so it may not be necessary to excise a large part of the cervix. Using a laser to destroy the abnormal cells can effectively treat the CIN and yet preserved the function of the cervix for future pregnancy.
Numbing medicine will be applied to the cervix beforehand so you don’t have to worry about pain. The laser beam also causes little to no damage to healthy cells, thus recovery is fast.
This is another procedure that can be used to destroy pre-cancer cells on the cervix. It uses a heated probe applied to the cervix for about 1-2 minutes. No anaesthesia is required.
This is usually used during the pre-cancerous stage, where abnormal cells have only been found on the surface of the cervix.
This is the usual treatment for early-stage cervical cancer. In very early-stage cancer, a simple hysterectomy that involves removing the womb and cervix, and occasionally the fallopian tubes and ovaries, may suffice.
In advanced stage 1 and some early stage 2 cervical cancer, a radical hysterectomy involves the removal of the cervix, womb, top of the vagina, surrounding tissue, lymph nodes, fallopian tubes, and sometimes the ovaries.
This is usually only suitable if the cancer is diagnosed at a very early stage and offered to women who still want to have children in the future and want their wombs preserved.
During the procedure, the cervix and upper part of the vagina are removed, leaving the womb intact, which will then be reattached to the lower part of the vagina.
It must be noted, however, that the surgeon cannot guarantee that you will definitely be able to get pregnant in the future, and even if you do, you will have to deliver via caesarean section.
This is a major procedure that is only recommended when the patient suffers from recurrent cervical cancer; and if the cancer has returned, but has not spread past the pelvis.
This procedure involves the possible removal of the vagina, bladder, rectum, and the cancer itself. Stomas are then created to allow you to pass urine and bowels out of your body into colostomy bags.
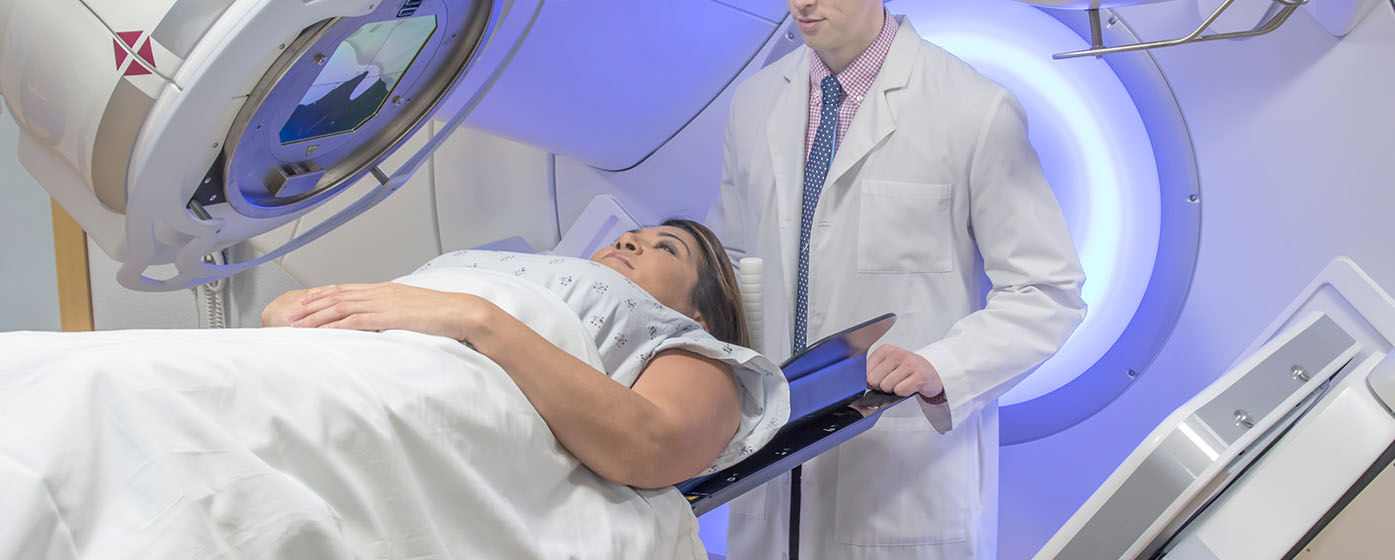
This may be used on its own or together with surgery recommended for early-stage cervical cancer. In advanced-stage cervical cancer, it may be used concurrently with chemotherapy.
High-energy waves may be beamed directly into the pelvis in order to destroy cancerous cells; or a radioactive implant may be placed next to the tumour through the vagina.
Lasting an average of 5 to 8 weeks, radiotherapy aims to destroy cancer cells, though it inevitably also affects some nearby healthy cells. These side effects may be temporary or permanent, and it is best to seek your doctor’s advice on your options.
Chemotherapy can either be combined with radiotherapy or used on its own. It is usually administered through an intravenous drip to destroy cancer cells. However, as with radiotherapy, chemotherapy often inevitably affects some neighbouring healthy cells; thus, side effects are common. However, upon the completion of chemotherapy, most side effects should subside.
Whether it is pre-cancer, early-stage cancer, or advanced-stage cancer, our medical team—comprising a gynaecologist and dedicated nurses—will work closely with you to provide personalised treatment and rehabilitation plan and emotional support for you from the moment you enter our care until you are discharged with a new lease on life.
Most cervical cancer patients will experience pain at some point, either as a result of the disease itself or due to the treatments they undergo. Common types of pain associated with cervical cancer include:
Fortunately, there are various medications available that can control and alleviate cervical cancer pain. These include:
Though necessary, cervical cancer treatments can come with side effects. Here are some common ones and how to manage them:

Our Colposcopy Specialist,
Consultant Obstetrician, Gynaecologist and Colposcopist
MBBS (Dublin), MRCOG (UK), FAMS (Singapore)
For over 20 years, Dr Quek Swee Chong has been providing comprehensive, evidence-based treatments for cervical cancer in Singapore, including colposcopy, hysterectomy, and laser surgery, to effectively address the needs of his patients.
He has held numerous leadership roles as well as research contributions in the field of cervical cancer, both locally and internationally. As a dedicated cervical cancer specialist in Singapore, he combines his extensive expertise with a compassionate approach to deliver optimal outcomes and improved quality of life for those under his care.