
Once a leading cancer among women and a leading cause of cancer death around the world, cervical cancer rates have fortunately since plummeted; though much more can be reasonably done to bring the numbers even lower.
Cervical cancer is now recognized as a highly preventable and treatable (in the early stages) cancer, partly because of the slow-progressing nature of the development from a HPV infection to cervical cancer (often up to 10 years or more); and partly because of the plethora of simple and effective screening options widely available:
Other lifestyle choices to reduce the risk of cervical cancer include limiting the number of sexual partners you have, using a condom and not smoking.
One of the most useful things about the Pap smear is how it can detect cell changes and abnormal cells in the cervix before they turn cancerous; allowing your doctor to either engage in watchful waiting (since most cases clear up on their own within two years, thanks to our immune systems), or perhaps opt to remove these cells pre-emptively before they possibly progress into cancer.
Though the HPV test does not indicate whether a woman has cervical cancer or not, it does indicate whether HPV is present or not; which can prompt the gynaecologist to conduct further testing, closer monitoring or treatment of any abnormal cells.
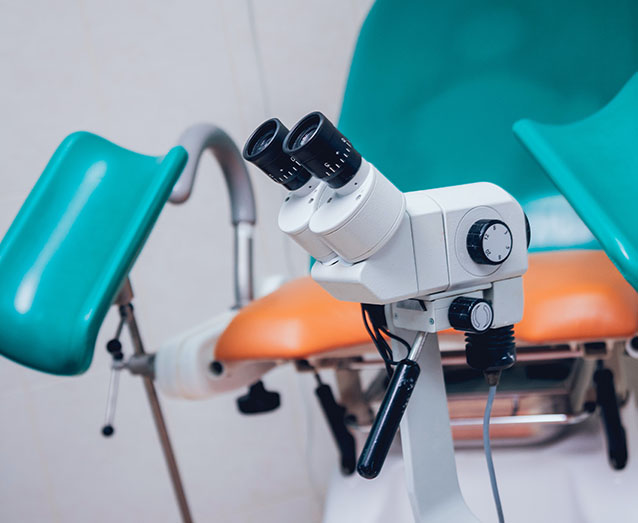
A colposcopy is a procedure used to examine the cervix in greater detail through a special magnifying instrument known as a colposcope; and it may be recommended if a Pap smear, HPV test or pelvic exam uncovers any abnormalities. If abnormal areas are identified, a small sample of tissue (a biopsy) may be removed for closer examination. The procedure generally takes no more than 10 minutes, and is performed in the clinic without the need for any anaesthesia.
If any of your tests uncovered abnormal cervical cells, particularly after a colposcopy, don’t worry—most women don’t uncover cancer at this point (if timely screenings have been adhered to), plus mild abnormalities don’t always need to be treated immediately.
Cervical cancer screening is generally successful because abnormal cell changes can happen many years before progressing into cancer, making early detection and intervention all the more effective.
If, however, treatment is needed, the goal will be to remove the abnormal cells while preserving as much normal tissue as possible. There are many well-established ways to do this.

To that end, he serves on the board of the International Federation of Colposcopy & Cervical Pathology, and his extensive research and humanitarian work centre around HPV and cervical cancer as well.