

Dr Quek Swee Chong Consultant Obstetrician, Gynaecologist and Colposcopist MBBS (Dublin), MRCOG (UK), FAMS (Singapore)
Regular cervical cancer screening plays an important role in protecting women's health. Cervical cancer often develops slowly and may not cause noticeable symptoms in its early stages. As such, it is vital for doctors to detect abnormal cervical cells early on, so that they can begin treatment before these cells develop into cancer.
In Singapore, national screening guidelines recommend different screening methods and intervals depending on a woman's age and risk factors. Understanding when to begin screening, how often to undergo testing and what each test involves can help women take a more proactive and well-informed approach to their reproductive health.
Cervical cancer screening serves as a preventive health measure that helps detect early cellular changes in the cervix before cancer develops. This screening plays an important role in women's health for several reasons:
Cervical cancer screening is recommended for women in different risk groups. The screening schedule may vary depending on individual health factors and medical history.
Women aged 25–69 who have ever been sexually active are considered to be at an average risk level of cervical cancer. Regular screening can help detect early cervical cell changes and conditions such as HPV before they progress into more serious conditions.
Women with weakened immune systems, such as those living with HIV or who have undergone an organ transplant, may be more vulnerable to persistent HPV infections. More frequent sessions of cervical cancer screening is often advised, as symptoms and pre-cancerous development are more likely to appear.
Women with a history of abnormal Pap smear or HPV test results, or previous cervical pre-cancer, may require closer follow-up. Healthcare providers may recommend a more frequent screening schedule to monitor for recurrence or new cervical changes.
As per guidelines from the Health Promotion Board (HPB) and the National Cervical Cancer Screening Programme in Singapore, the recommended screening method and frequency vary according to a woman's age.
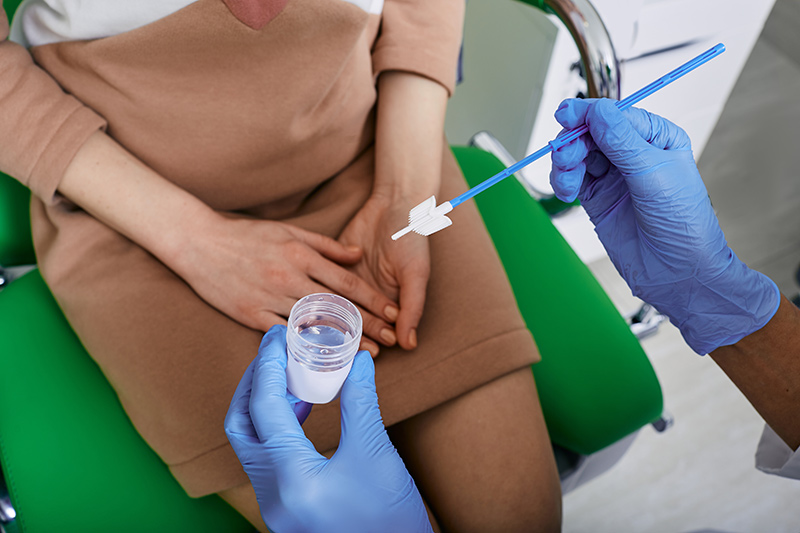
For women aged 25–29 years old, screening is performed using a pap smear, typically with liquid-based cytology, every 3 years. This test involves collecting cervical cells to examine them for abnormal changes.
In this age group, many HPV infections are temporary and resolve without treatment. Screening at three-year intervals allows appropriate monitoring while reducing the likelihood of unnecessary follow-up procedures. If results remain normal, screening can continue at this interval.
For women aged 30–69 years old, HPV primary screening is recommended every 5 years. This test detects the presence of high-risk HPV strains that are responsible for most cervical cancers. Sample collection may be performed by a clinician or through self-sampling, which may offer greater privacy and convenience for some women.
In this age group, persistent high-risk HPV infection is more strongly associated with the development of cervical cell changes. A 5-year interval is considered appropriate because clinically significant infections are more likely to be detected within this timeframe.
In some cases, HPV co-testing may be advised. This approach combines the HPV test and Pap smear in a single screening session. It may be recommended for selected women based on their individual risk factors and their doctor's clinical assessment.
An abnormal cervical screening result does not necessarily mean that cervical cancer is present. In many cases, screening detects early cellular changes or precancerous lesions that can be monitored or treated before they develop into cancer. Further tests are usually recommended so that doctors can assess the cervix more closely and determine the appropriate treatment plan.
Depending on the screening findings, the following steps may be advised:
If Pap smear or HPV test results are abnormal, a doctor may perform a colposcopy, a procedure that uses a magnifying instrument to closely examine the cervix and identify abnormal areas of tissue. In some cases, a biopsy may be taken during the procedure to confirm whether abnormal cells are present.
For mild abnormalities, doctors may recommend repeating the Pap smear or HPV test at shorter intervals. This allows them to monitor whether the abnormal cells resolve on their own or require further treatment.
If precancerous changes are confirmed, treatment may be recommended to remove the abnormal tissue and prevent progression to cervical cancer. Common procedures include:
These treatments aim to remove abnormal cells while preserving as much normal cervical tissue as possible. With timely follow-up and appropriate management, many abnormal screening findings can be treated effectively before they develop into cervical cancer.
You should consult a doctor about cervical screening if you:
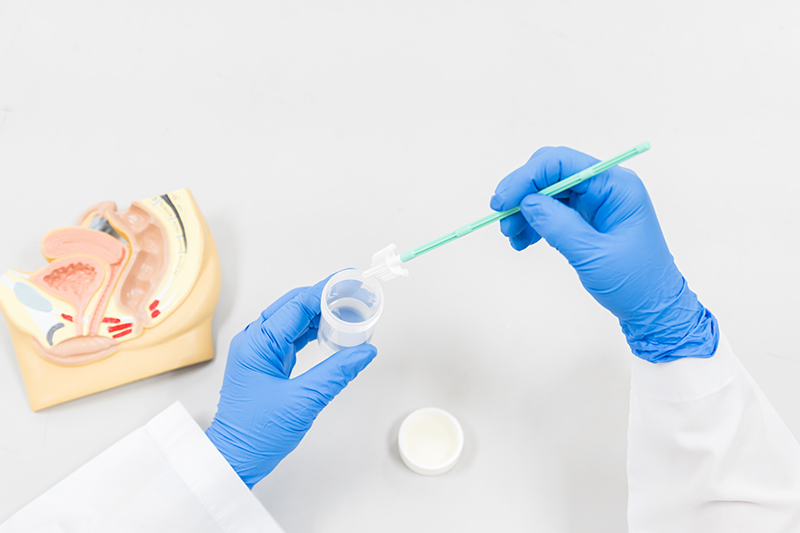
Cervical cancer screening remains an important component of women's health in Singapore. Regular screening is an important preventive measure that gives doctors the opportunity to detect abnormal cervical cell changes early, before they develop into cervical cancer. Early detection allows appropriate monitoring or treatment to be started promptly, which can help reduce the risk of disease progression.
At SC Quek Gynaecology, cervical cancer screening is guided by Dr Quek Swee Chong, a consultant obstetrician, gynaecologist and colposcopist with a clinical focus on cervical cancer prevention, detection and management. Dr Quek provides screening in accordance with current cervical cancer screening guidelines in Singapore, with care centred on clear communication, patient comfort and recommendations tailored to each patient's health profile.
If you are due for cervical cancer screening or would like guidance on the appropriate screening schedule for your age and risk factors, contact us today to arrange a consultation.
Yes. While the HPV vaccine provides strong protection against the most common high-risk HPV types, it does not cover every strain. Regular cervical screening remains important, as it works alongside vaccination to detect any early cervical changes and support long-term cervical health.
Women over 65 who have had consistently negative results and no history of significant cervical pre-cancer may discuss with their doctor whether screening can be discontinued.
Cervical screening is generally safe during pregnancy when performed with appropriate clinical guidance. If you are pregnant or planning to conceive, discuss the timing of screening with your doctor.
Yes. Cervical cancer screening is recommended even if you do not have symptoms. Early cervical cell changes and HPV infections often do not cause noticeable symptoms, which is why regular screening is important. Screening allows doctors to detect abnormalities early and manage them before they develop into more serious conditions.

Our Colposcopy Specialist,
Consultant Obstetrician, Gynaecologist and Colposcopist
MBBS (Dublin), MRCOG (UK), FAMS (Singapore)
With vast expertise in obstetrics and gynaecology, Dr Quek specialises in colposcopy, a critical procedure for the early detection of cervical cancer and its precursors. His experience encompasses diagnosing and treating cervical dysplasia and cancer, utilising advanced techniques to ensure comprehensive patient care. Over the years, he has contributed significantly to the field through clinical practice and patient education, focusing on preventive measures such as HPV vaccination and regular screenings to reduce cervical cancer incidence.